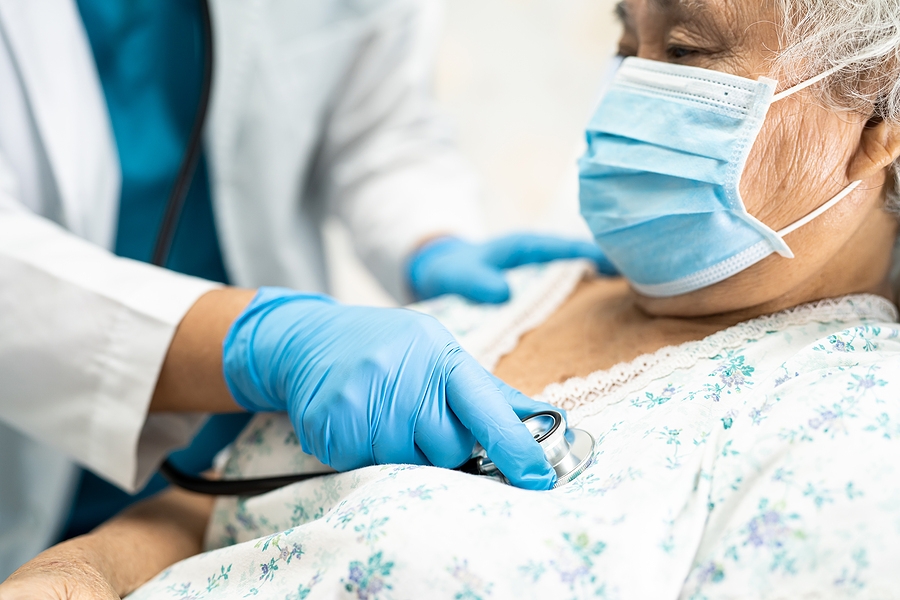
Why are we more susceptible to COVID-19 as we age?
A major reason for older folks having a higher susceptibility to COVID-19 than younger people is comorbidity. If you have comorbidities, meaning two or more negative health conditions at once, including COVID-19 and diabetes, or hypertension or cardiovascular diseases, you have a higher risk of complications and mortality due to COVID-19. Having both COVID-19 and increased blood clot activity occurring frequently in hypertension, diabetes, and cardiovascular disease; enhances the virulence and infectivity of the SARS-CoV-2 virus by cleaving to and aggravating its spike proteins.
Also as we age, the immune system becomes less effective, or immuno-compromised, and coagulopathy, defined as excessive bleeding and/or blood clotting, can occur. These increased risks of coagulation from excessive bleeding and blood clotting, plus a declining immune system, makes us more vulnerable as we age to pathogens, including the COVID-19 disease from the SARS-CoV-2 virus.
You have probably heard of a major risk in COVID-19 being cytokine storms. In a cytokine storm, “the innate immune system causes an uncontrolled and excessive release of pro-inflammatory signaling molecules called cytokines. Normally, cytokines are part of the body’s immune response to infection, but their sudden release in large quantities can cause multisystem organ failure” [Wikipedia].
Did you know one in two who perish from a cytokine storm are over 60? [Thachil J, Agarwal S. https://doi.org/10.1111/anae.15141]. In other words, as you get older, you become more vulnerable to COVID-19 due potentially from coagulopathy and cytokine storms.
Another potential negative from aging is Alveolar macrophages primarily in the lungs increase as we age, but their ability to convert between pro- and anti-inflammatory states needed to fight COVID-19 are significantly reduced. This accelerates COVID-19 in its early stages in the elderly, and in advanced stages, can cause excessive lung damage. This gradual decline in immune function is technically called immuno-senescence. The immuno-senescence of the adaptive immune system in the elderly also contributes to progression to severe COVID-19.
Exactly what happens as we age to our immune systems? A decline in neutrophil immune cell activity as we age causes these cells to lose their ability to migrate to sites of infection and kill infected cells including from viruses. In immuno-senescence, impairment of both forms of immunity, innate and adaptive, occurs. The immune system is negatively impacted by ineffective pathogen recognition, lessened macrophage activation, and reduced natural killer (NK) cell cytotoxicity. [Mueller AL, McNamara MS, Sinclair DA. Why does COVID-19 disproportionately affect older people? Aging (Albany NY). 2020;12(10):9959–81].
A chronic increase in systemic overactive, but ineffective, inflammation, is known as inflammaging. Inflammaging is a major driver for increased cytokine storms occurring in aged individuals, especially with COVID-19, and made worse by obesity, poor diet, poor oral health, microbial dysbiosis, and sedentary lifestyle [Thachil J, Agarwal S. 2020. https://doi.org/10.1111/anae.15141].
The inflammaging process in older patients contributes to the rapid progression to cytokine storms, whose key player is NLRP3. NLRP3 is the major protein component of the inflammasome responsible for inflammatory responses and is present in large amounts in older individuals. Also influencing are a decline in the production of fresh naïve T cells, T cell metabolic dysfunction, and weaker activation of T cells that all contribute to enhanced immune vulnerability of the aged to COVID-19.
Frankly speaking, we cannot stop aging but we can adopt a lifestyle that promotes good health and a quality life. Begin a healthy lifestyle young to avoid many of the factors of aging that contribute to being more vulnerable to not just COVID-19, but most pathogens that seek to take your health.
Proper diet, adequate rest, good hygiene including washing hands, moderate exercise, no smoking or illegal drugs, stress management and oral supplementation when appropriate all reduce the negatives of aging and thus the vulnerability of senior citizens to COVID-19.